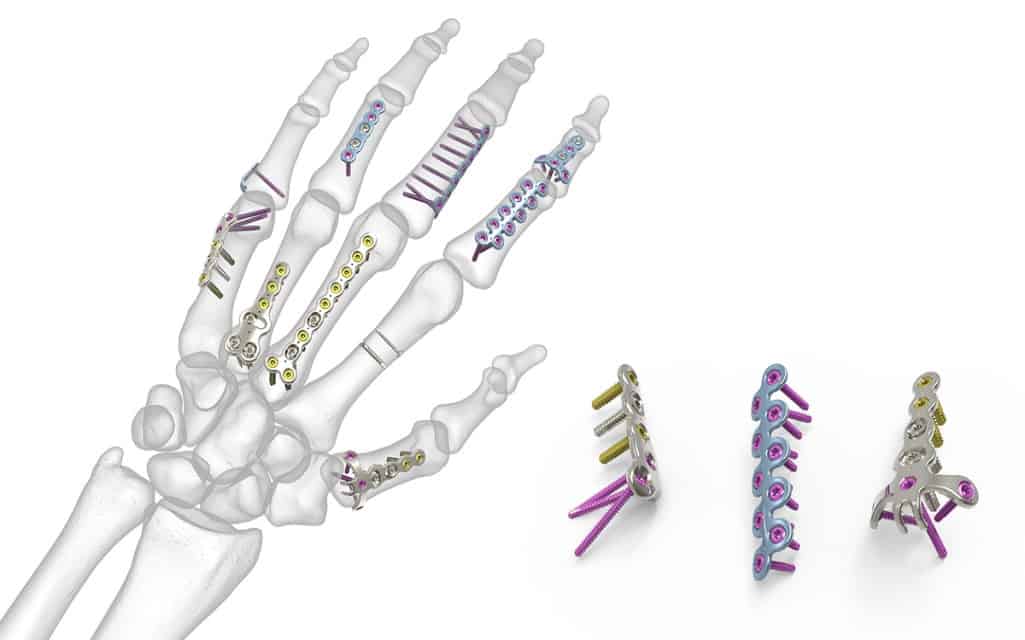
A wide variety of locking plates for hand fracture surgery are available. But for hand fractures particularly with serious bone comminution, intra-articular fractures, segmental bone loss, and open fractures, a miniature plate system is very useful. It facilitates rigid fixation to reduce pain and edema which allows early mobilization exercise. This can keep the restrictive scarring to a minimum which can obstruct the gliding of tendinous structures all around the phalanges.
Some earlier studies show that complications of early stainless steel mini-plate fixation result in complications such as pain, impingement of the plate, infection, and tendon adhesions. The titanium mini-plate system has also revealed some complications when applied in complex injuries of the hand. However, breakage of titanium screws while removing and inserting the screw and the breakage of titanium plate due to delayed union or non-union were common.
Furthermore, obvious adhesion between the tendon and the titanium plate was observed during the secondary operative procedures which include removing the plate and screws, tenolysis, and capsulotomy
The use of stainless steel implants in place of rough titanium implants is preferred in hand fractures because the initial soft tissue injury and the injury from the surgical dissection can add to the adhesion, it is also associated with the surface topography of the titanium implant which is neither smoothed nor polished. The mid-axial approach and lateral placement of the plates or screws for all proximal phalangeal fractures were adopted to move the surgical injury zone away from the extensor mechanism. As per literature, it could decrease the risk of tendon adhesions and a decrease in stiffness.
Freeland et. al. 24 found that unilateral excision of the lateral band and oblique retinacular fibers of the metacarpophalangeal joint extensor expansion could lessen the risk of post-operative adhesions, intrinsic tightness, and tissue irritation when the plate was inserted on the proximal phalanx laterally.
The etiology of the finger stiffness included related injuries of soft tissue, like extensor tendon injury, bony comminution, and delayed mobilization exercise from bracing that resulted in adhesion of tendon and secondary joint contracture. The passive motion could not be sustained by the strength of the stainless steel miniature plate particularly in case of comminuted fracture, so the stainless steel 2.0-mm LCP system was used to provide more stable fixation for the hand’s comminuted fractures to provide early passive mobilization exercise and aggressive restoration.
The AO Foundation has given the same indications for 2.0 mm Locking Compression Plates in hand fractures surgery as for the conventional plates. Though, it is useful especially for managing the comminuted fractures of metacarpals and proximal phalanges, arthrodesis, periarticular fractures, and mal-union which require corrective osteotomy because these locking plates provide better stability in case of comminuted fracture. Moreover, it provides better stability without the application of axial compression as in the case of conventional plates. It works as an internal fixator which requires a minimum of two locking screws on each side of the fracture. More strength to the construct of bone-plate is added by the fixed-angle locking plate screws through locking mechanism to attain more reliable fixation and better angular stability as compared to the conventional plate that largely depends on the frictional resistance between the plate and bone to attain the complete stability. This is important for aggressive rehabilitation protocol.
Read More: How To Look Younger Without Getting Invasive Plastic Surgery
Additionally, the blood flow of the bone beneath the LCP will not be at risk. It also can be used in cases of poor bone quality, bone loss, and poor bone stock. The pin tract problem that is common in external fixator or percutaneous Kirschner wires does not occur in it. It is mainly useful for periarticular fracture patterns as two locking screws on the juxta-articular fragment will be strong enough.